
At the University of North Carolina School of Medicine, it’s $495,000 a year.
The figure comes from this recent paper in Medical Science Educator.
If you want to get a surprisingly frank, behind-the-scenes look at how Step 1 Mania affects the medical school curriculum, I’d highly encourage you to read the whole paper. But for the TL;DR crowd, let me summarize the high points here.
Background
Our story takes place at the University of North Carolina School of Medicine – an elite U.S. medical school ranked #1 in Primary Care and #23 in Research by U.S. News & World Report.
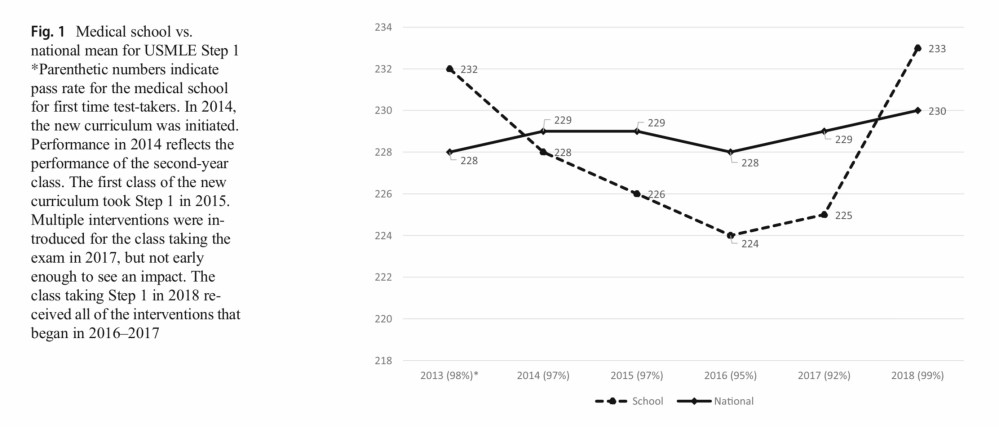
For many years, UNC faculty chose not to “overemphasize” preparation for USMLE Step 1. Their students did well on the test – with a class average slightly better than the national mean – and they had good success in the Match. (In 2013, for instance, the UNC Step 1 mean was 232, vs. a national mean of 228.)
Then, in 2014, the school changed to an integrated, organ-system based curriculum.
Faculty were aware that making this change might lead to a drop in their Step 1 average.
Having consulted with other medical schools who changed their curricula, we anticipated that USMLE Step 1 scores might drop somewhat and they did, while the national mean continued to rise.
In the era of Step 1 Mania, this created a big problem. By 2016, the average UNC Step 1 score was 224, 4 points below the national average.
And this problem did not escape the notice of administrators. Soon, faculty were called upon to tool up and join the Step 1 arms race and get those scores back up. Over the following several years, the school made the following changes:
1) Begin using NBME exams
Instead of using faculty-written questions for exams, UNC began purchasing questions from the NBME. This “exposed students to the rigors and format” of Step 1 for their UNC courses.
Total cost: $100,000/year
(N.B. – I’ve written before about how lucrative this particular revenue stream has become for the NBME.)
–
2) Providing Step 1 prep material
To ensure that all students prepared adequately for the Step 1 exam, UNC purchased both the UWorld Step 1 Qbank and USMLE-Rx for all students.
Total cost: $150,000/year
–
3) Hiring faculty
The school also hired additional faculty to shepherd the students through Step 1. Two faculty members were given salary support (totaling 0.75 full-time equivalents, or FTE) to teach test-taking skills and provide one-on-one test-taking counseling with medical students. (The latter service was used by over half the students in the class.). Additionally, a third faculty physician received 0.5 FTE for “analyzing performance metrics” to improve Step 1 performance.
Total cost: $245,000/year
–
4) Re-calibrating the curriculum
Here, let me quote from the paper, with my emphasis added:
[A]n audit… was undertaken to evaluate content discrepancies between our curriculum and “high-yield” Step 1 topics. A commercial review book popular with medical students was used to detect co-alignment and deviation between the content of our curriculum and USMLE Step 1.
Total cost: Nominal… beyond the public admission that a top-flight U.S. medical school uses First Aid for the USMLE to determine the content of its curriclum.
(And before I move on, let me be clear: nothing here is meant to impugn UNC. They’re not the bad guys in this story, and I truly applaud the authors of this paper for being so forthright about their experience. Moreover, the medical school where I teach also purchases UWorld for students and uses NBME exam questions – and I’d be willing to wager that every other medical school is doing some of these same things to chase Step 1 scores.)
–
Results… at a price
The action plan above worked.
By the time the full plan had been implemented, the school’s mean Step 1 score had jumped 9 points, and UNC students were again scoring above the national USMLE Step 1 average.
But all of this stuff – the extra faculty, the NBME exams, UWorld, etc. – it wasn’t cheap. The total cost for the measures above is $495,000/year – or $55,000 per point of Step 1 increase.
Importantly, these costs are described in the paper as being incurred by the medical school. From an accounting standpoint, that’s true. But rest assured that no medical school is going to pay $150,000/year for UWorld or USMLE-Rx out of charity. Those costs are ultimately going to be borne by the students themselves.
And if that $495,000/year cost was split equally among each of UNC’s entering class of 192 students, it would increase the cost of tuition by $2,578.13.
Is it worth it?
From the school’s standpoint, it’s hard to argue that it wasn’t. (In fact, I’ll bet there are many medical schools who would happily pay several multiples of $55,000 to increase their students mean Step 1 scores by a few points.)
We have chosen to live in a world where the Step 1 score is the coin of the realm. Had UNC administrators chosen a different path after the implementation of their new curriculum – had they said, “Damn the students’ Step 1 scores! Full speed ahead!” – both the school’s reputation and its students would have suffered.
The real question is, are we all okay with this? Are we all cool with continuing to worship the biggest false god in medical education?
Or, as the authors suggest, is it time to take action?
We offer this case study as an example of unreported costs of the “Step 1 Climate” and the substantial efforts made in preparation of an examination whose meaning is being misused by the national community of medical education leaders – to the detriment of student development. We support Haertel’s recent call to action imploring educators and stakeholders to stop the use of exams for purposes other than their original design. We add to that call, noting costs and threats to validity in hope of encouraging those responsible for the future of our profession to take action.