
As the year draws to a close, it’s time for all the prognosticators and pundits make their predictions for the coming year. Obviously, I don’t want to miss out. So here are the Sheriff of Sodium’s predictions – nay, prophecies – for 2022.
–
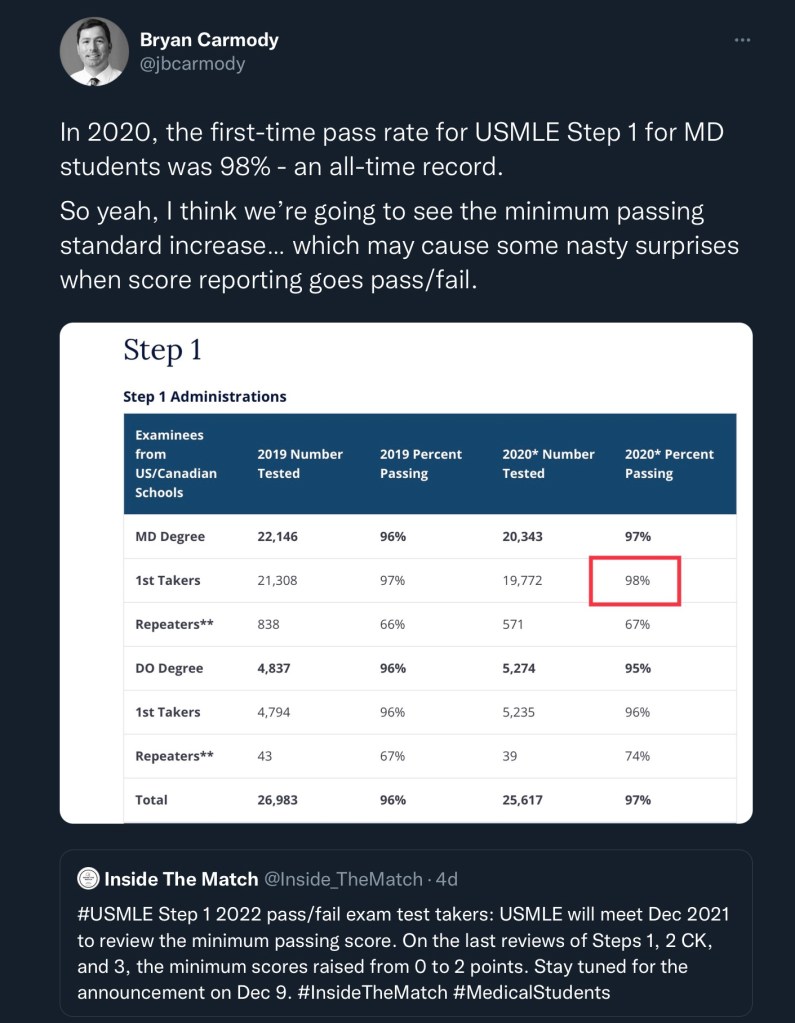
The USMLE Step 1 minimum passing standard will increase
Oh wait – that already happened.
Well, whatever. This is my website, and I predicted it – so even if it happened in December 2021, I’m still taking credit for it in my 2022 predictions. So there.
–
Interviews for the 2022-2023 residency cycle will be virtual
I say this for two reasons.
One is that, in case you haven’t heard, COVID-19 isn’t going anywhere. So if you thought that 2022 would be substantially different than 2020 or 2021 in almost any way, I think you’ve got another think coming.
But second – and more relevant to residency application in particular – is that virtual interviews work, and both applicants and programs seem to like them. Everyone, I think, realizes that there is something lost when interviews are virtual – but that something comes at a cost that we’re not yet willing to pay. For reasons including expense, equity, efficiency, and inertia, I’ll be very surprised if the 2022-2023 is not virtual.
–
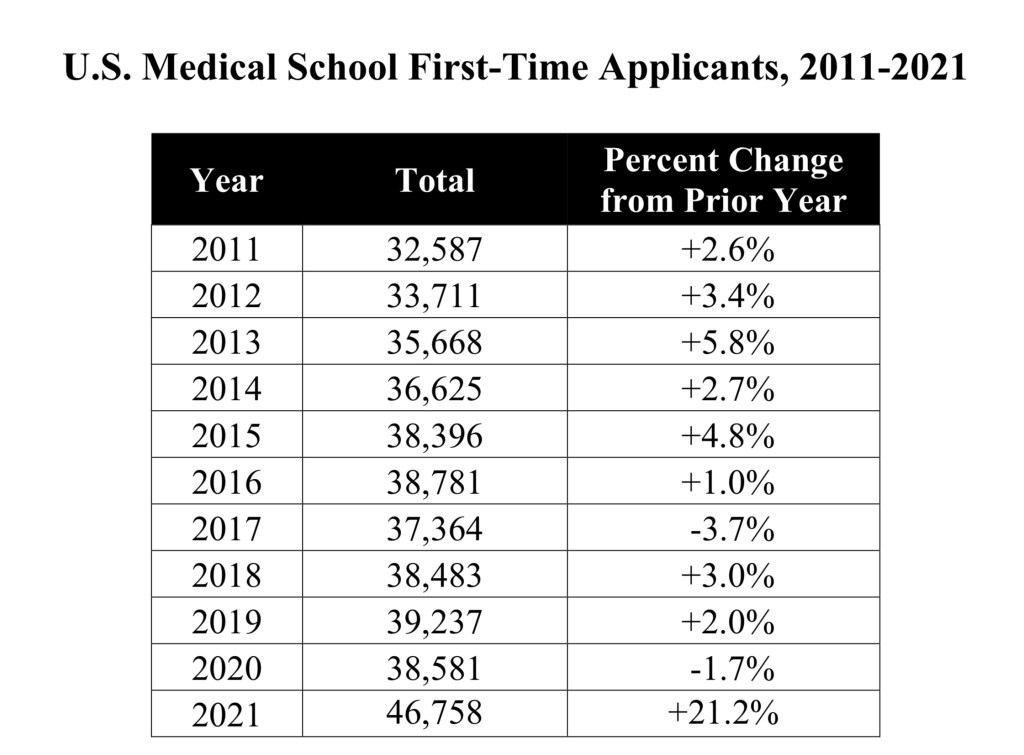
The AAMC and AACOM will announce a decrease in medical school applicants
Remember last year when the AAMC was trumpeting the “Fauci effect” as an explanation for sudden surge in medical school applicants last year? Isn’t it curious, then, that although both Dr. Fauci and COVID-19 are still alive and well, we haven’t heard a peep about the Fauci effect this year?
I’ve heard rumors that medical school applications are down significantly – maybe back to 2019 levels. In contrast to last year, though, neither the AAMC nor AACOM have chosen to share preliminary application data.
But once the season is over, the final data will be released… though if applications are down, you can expect that data release to occur without the same fanfare and glib quotations that accompanied the preliminary data release last fall.
(It’s worth noting that the premise of the “Fauci effect” was implausible from the very beginning. To get into medical school these days requires years of planning and resume-padding. It strains credulity to believe that there was an enormous but untapped reservoir of qualified applicants who just so happened to have taken the MCAT and completed all academic pre-requisites, but just didn’t feel inspired to apply until they saw Dr. Fauci on the television. In reality, the surge in applications probably has more to do with ‘gap year’ opportunities drying up.)
–
The Match Rate will increase

The 2020-2021 residency selection cycle was disrupted by COVID-19 and all that came along with it. But even then, Match rates dropped only slightly. Graduating MD students matched at a 92.8% rate, while 89.1% of graduating DO students, 59.5% of U.S. citizen international medical graduates (IMGs), and 54.8% of non-U.S. citizen IMGs successfully matched.
My prediction is that the match rate for all groups will rebound slightly this year.
(Of course… if I’m wrong… and lower Match rates become the new normal, it should spark some serious debate about whether the cause can rightfully be attributed to COVID-19, or whether it might more reasonably be ascribed to a congested system under strain from Application Fever.)
–
Healthcare worker shortages will persist
And no, this is not a prediction about COVID-19. Since early 2020, I’ve tried hard to stay in my lane, listen to real experts, and avoid the temptation to become a pandemic prognosticator just because I have a social media platform.
But although I don’t claim to know anything about pandemics, I do know some things about our health care system. And the way that most people talk about health care worker shortages is not the way that these shortages are viewed by the people who make the most important decisions about them.
To a patient, having to receive critical care in the emergency department because there are no ICU beds available is definitely a nonideal outcome. But in a purely economic sense… well, this is a more efficient and remunerative situation than having unused ICU beds, right?
To a nurse struggling to care for multiple critically ill patients simultaneously, it’s easy to perceive that there’s a major problem with staffing. But again, in an economic sense, where’s the problem? This is maximizing efficiency! So what if people burn out early? As long as they don’t burn out faster than you can replace them, it’s still a net positive. If you’re an administrator, once your team has shown that they can do more with less, it’s hard to ever justify returning to doing more with more.
For many doctors, nurses, and other healthcare professionals, their job is more than just a paycheck. But for those who lead the organizations responsible for the direction of our health care system as a whole, it’s all just economic activity.
In my opinion, worker shortages are here to stay. And the culprit isn’t the virus, or the unvaccinated, or anything else other than the extractive mindset of the leaders of a system that has been increasingly optimized to function primarily as an economic engine.
–
We’ll hear more about an interview match
At this point in its history, there’s not much that threatens the National Resident Matching Program.
The Match is a cultural rite of passage, and the NRMP provides a service that is valued by the majority of programs and applicants. Moreover, their “All In” policy and Congressional antitrust protection make it difficult to imagine a world in which residency selection occurred without the NRMP.
These days, the single biggest threat to the Match is Application Fever – because worsening congestion in the residency application marketplace makes it increasingly tempting for programs to consider operating outside the Match. And if this occurred, it could make the whole Match unravel.
In December, a group of authors including NRMP Board member and Nobel laureate Alvin Roth published a paper that proposed a novel solution to ease some of the congestion in the residency application process: an interview match.

The idea is simple. Applicants would apply to programs as usual – but when they did, they’d rank programs in their order of interest, while programs did the same. Then, the NRMP would use its matching algorithm to assign interviews based on mutual interest from programs and applicants. (The final ranking process and Match would occur after the interviews and proceed just as it does now.)
The intent of such a system is to reduce the number of “low value interviews” that programs conduct and applicants attend. But in my opinion, an interview match is at best a half-measure – and more likely, its implementation would cause several complications and unintended consequences.
Still, because of the credentials of the authors and the strain of Application Fever, I expect we will hear this proposal being seriously considered in 2022. I’ll hold my fire for now – but if this idea does start to catch on, come back for an in-depth analysis.
–
COMLEX-USA Level 2-PE will return
Back in the first few months of the COVID-19 pandemic, we saw the USMLE rapidly spin down their Step 2 CS testing operation, releasing paid staff and leasing out their real estate.
In contrast, the National Board of Osteopathic Medical Examiners (NBOME) worked hard to keep their Level 2-PE exam afloat: they took out two Payroll Protection Plan loans and even announced plans to open a new satellite testing center near Fresno, CA.
It took a while to convince me that USMLE Step 2 CS was really dead – but at this point, I think it is: the USMLE has been conducting market research other ways to leverage their expertise in standardized patient examinations.

In contrast, I think the Level 2-PE has just been sleeping… and it’s hard to imagine the NBOME walking away from all they’ve invested in their test. This spring, I think they’ll announce plans to reinitiate the exam for the Class of 2023.
This will, of course, open up multiple cans of worms. Why should the Class of 2023 have to take the Level 2-PE when the classes of 2021 and 2022 didn’t? Why should DO students have to take a national clinical skills exam when MD students are no longer required to do so? So pop your popcorn, and look forward to a re-enactment of the old War Against Step 2 CS.
–

The NBME will be back in court
From time to time, and as part of the service I provide to readers of this website, I peruse the public records of lawsuits involving parties of interest to those in medical education. The National Board of Medical Examiners (NBME) is a frequent defendant (most commonly in lawsuits filed by examinees who allege they were wrongfully denied testing accommodations to which they should have been entitled under the Americans with Disabilities Act). But there’s one lawsuit in particular involving the NBME that I’ve been following over the past year… and I don’t think we’ve seen the last of it yet.
The general facts of the case are these:
The plaintiff was a resident physician at a prestigious institution who struggled to pass USMLE Step 3. He took the test and scored a 192, below the passing standard of 196. So he took the test again eight months later – but again failed, this time with a score of 178.
What happened next? Well, here accounts diverge.
According to the plaintiff, he received an e-mail from the NBME informing him that one of his Step 3 attempts had been erroneously reported as a failure. The new score report he received showed his score to be 199. By his account, he dutifully passed on the new score report to the state licensing authority and received a license.
According to the NBME, no such e-mail was ever sent.
And so, in a disciplinary hearing before the USMLE’s Committee for Individualized Review (CIR), the examinee was found to have engaged in irregular behavior and the state board was informed that it had received a fraudulent score report – throwing the doctor’s license, job, and visa sponsorship/immigration status in jeopardy. He therefore filed suit against the USMLE and its corporate co-sponsors, the NBME and the Federation of State Medical Boards.
In the administrative and legal proceedings, the NBME has provided multiple lines of evidence supporting their position that the score report was fraudulent. However, the plaintiff has countered by retaining with an national computer expert, and have asserted that the expert’s forensic evaluation of the e-mail concluded that it was authentic.

So far, the court has made no determination about the veracity of the e-mail or score report. But the plaintiff did win a preliminary victory: the court vacated the USMLE’s disciplinary decision, finding that they did not adhere to their own procedures for the CIR hearing (specifically, by withholding their own evidence on the forensic evaluation of the e-mail and score report). For the time being, the court’s injunction allows the plaintiff to keep his medical license and forestalls deportation proceedings, with a court-ordered do-over of the USMLE CIR hearing scheduled to occur in 2022.
The CIR’s deliberations and decisions are private – but regardless of the outcome of that hearing, I think we’ll hear more about this case in the courts. If the plaintiff prevails, I expect he’ll pursue the USMLE for costs and damages. If he fails, he’ll have no other option than a last-ditch legal remedy to salvage a medical career in the United States.
–
So stay tuned. I’ll make a point of revisiting this post at the end of 2022 to see how many of these prophecies come to pass.
Wishing all of you my very best for a happy and healthy 2022…
–The Sheriff of Sodium
YOU MIGHT ALSO LIKE:
Match Day 2021: Winners & Losers Edition